Why to Join Aesthetic Medicine
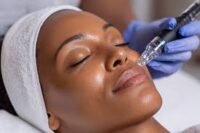
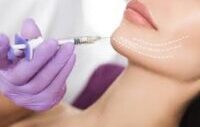
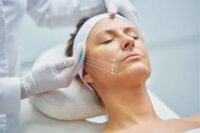
Your Career Pivot: Why Now is the Best Time for Physicians to Enter Aesthetic Medicine Many dedicated physicians are finding themselves at a career crossroads: burnout from endless charting, shrinking reimbursement rates, and a diminishing sense of professional autonomy. If you are seeking a medical field that rewards skill, offers flexible hours, and places you firmly in control of your income and practice environment, the answer is clear: Aesthetic Medicine.The aesthetic industry is experiencing massive, sustained growth, driven by patient demand for preventative care and a desire for non-invasive treatments. For a licensed physician, now is the optimal time to make the career pivot and capitalize on this booming market. 1.The Financial and Professional Freedom The shift from insurance-based medicine to cash-pay aesthetics offers several unparalleled financial benefits: Cash-Pay Model Aesthetic procedures are primarily patient-paid, eliminating the long delays, denials, and administrative costs associated with insurance billing. You control the pricing and the revenue cycle. High Profit Margin Injectables and devices often carry high profit margins, especially when inventory is managed efficiently Entrepreneurial Opportunity Physicians can start a practice part-time, scale quickly, and eventually become a Medical Director for multiple locations, creating passive income streams 2. Improved Work-Life Balance and Reduced Burnout One of the greatest appeals of aesthetic medicine is the opportunity to design a better life Elective Procedures Aesthetic treatments are generally elective, meaning no overnight calls, no emergency room visits, and no critical care required. Controllable Schedule You dictate your hours and patient load. Many successful aesthetic practitioners choose to work 3-4 days a week, dramatically reducing burnout and improving quality of life. Positive Patient Interactions: Patients seeking aesthetic improvement are typically healthy and motivated, leading to far more positive and satisfying clinical interactions. know more here about aesthetic medicine courses The Market Demand is Exploding and Maturing The aesthetic patient demographic is rapidly expanding beyond traditional borders: Generational Demand: Millennials and Gen Z are focusing on preventative ‘pre-juvenation,’ starting injectable treatments earlier than ever before. Male Aesthetics: The number of cosmetic procedures performed on men has seen dramatic growth, adding an entirely new segment to the market. Technological Advancements: The continuous release of safer, more effective devices (RF Microneedling, new laser systems) keeps the field dynamic and exciting. 4. Your Medical Background is Your Greatest Asset Patients prioritize safety, and your MD or DO degree is the ultimate differentiator: Safety and Trust: Your comprehensive medical training provides the foundation to manage complications, understand pharmacology, and safely integrate aesthetic treatments with a patient’s overall health profile. Anatomical Expertise: Compared to non-physician injectors, your in-depth knowledge of facial and body anatomy provides a superior basis for advanced injection and device techniques. The combination of professional autonomy, high earning potential, and a vastly improved work-life balance makes aesthetic medicine the most compelling pivot for physicians today. However, your clinical degree is just the starting point. Success in this specialized field requires dedicated, intensive training focused on aesthetic skill, safety protocols, and practice management. Ready to transition your career and launch a successful aesthetic practice? IAMAC Institute offers foundational and advanced certification programs designed specifically for physicians. View our course calendar and start your new, rewarding career today.
Why to Join Aesthetic Medicine Read More »